The History Of The Sexual Tipping Point® Model
The Sexual Tipping Point® (STP) model evolved from two decades of collaboration with my mentor, Helen S. Kaplan, MD, PhD at NY Weill Cornell Medicine in NYC. It was at Cornell’s Payne Whitney Clinic of the New York Hospital that Kaplan founded the first medical school–based sex therapy training and treatment clinic of its kind in the United States. Kaplan’s first book, The New Sex Therapy (1974), described that program’s outpatient treatment approach, which modified Masters & Johnson’s (1971) two-week pioneering residential program. As Kaplan’s book became the standard text for most students and medical institutions around the world, it had an impact on where and how people were treated for sexual problems both nationally and internationally. Kaplan brought the principles of multi-determinism and multilevel causality to sex therapy. Kaplan practiced a therapeutic eclecticism that anticipated current sexual medicine approaches that combine/integrate appropriate selection of medical and surgical treatments integrated with sex counseling that were first described by Althof, Leiblum, McCarthy, Rosen and myself, among others by the turn of the 21st century.
In Kaplan’s final book published the same year she died in 1995, Helen described a "psychosomatic" dual-control model of sexual motivation emphasizing “inhibition/excitation” processes. Kaplan’s concept was derivative of the work of Kupferman who in 1991 wrote, “All examples of physiological motivational control seem to involve dual effects—inhibitory and excitatory—which function together to adjust the system.” In response to that insight, Kaplan wrote, “Control of sexual motivation is no exception and also operates on such a “dual steering” principle… Once again, we can learn from the similarities between eating and sex” (Kaplan, 1995). Kaplan’s description and illustration of the dual control elements underlying human sexual motivation and sexual desire dysregulation anticipated Bancroft and his Kinsey Institute colleagues (Janssen, Graham, Heiman, Sanders, etc.) who later provided outstanding erudite articulation of dual-control theory, psychometrics, and comprehensive research (Bancroft et al., 2009). Additionally she foreshadowed the work of James Pfaus’s (2006) concepts of satiation of appetite being related to satiation of sexual desire as a theoretical mechanism to explain Hypoactive Sexual Desire Disorder. An artist by training, Kaplan had sketched a cartoon in that last volume that foreshadowed the current digital graphics developed for use in the STP model, which can be found on the mapedfund.org website.
Adapted with permission from Kaplan HS, The Sexual Desire Disorders. Dysfunctional Regulation of Sexual Motivation. Brunner-Routledge (Taylor and Frances, London, 1995: p. 15 (Fig. 2)
Kaplan dedicated that final book to her two decade–long collaboration with all her colleagues in our weekly seminar at the Human Sexuality Program at Cornell. In 1995, I was appointed as the next Co-Director of that program and Kaplan’s sketch inspired me to refine my own mind/body ideas into the Sexual Tipping Point model, which would provide a visual heuristic that could depict the intra and inter-individual variability of all sexual function and dysfunction. The STP model can illustrate all etiological permutations including “normal” sexual balance, and is particularly useful for modeling combination and integrated sexual medicine treatments in an easily understood manner that can be used to explain risk/benefit for patients with sexual disorders.
The Sexual Tipping Point® name derived from a concept that was “in the air” at the end of the 20th century. In fact, with the publication of his book in 2000, Malcolm Gladwell made the concept iconic. While Gladwell wrote and lectured about social epidemics and other macro forces, such as viral marketing, I was more interested in individual uniqueness and the continuous variability of both interpersonal and intrapersonal factors from a biopsychosocial–cultural perspective. In particular he wanted to apply it to both sex therapy and to sexual medicine. To document and distinguish the differences between Gladwell’s exceedingly well-known views and his own, I sought and was awarded a trademark registration for his Sexual Tipping Point® concept by the U.S. Patent and Trademark Office in 2005.
The Sexual Tipping Point® represents the cumulative impact of the interaction of a constitutionally established capacity to express a sexual response elicited by different types of stimulation as dynamically impacted by various psychosocial-behavioral and cultural factors. An individual’s threshold will vary somewhat from one sexual experience to another based on the proportional effect of all the different factors that determine that tipping point at a particular moment in time with one factor or another dominating while others recede in importance. Besides illustrating all etiological permutations, including normal sexual balance, the Sexual Tipping Point model is particularly useful for modeling treatment and can easily be used to explain risk–benefit for patients with sexual disorders. In fact, the Sexual Tipping Point also allows for modeling of a variety of integrated treatments, including future medical and surgical interventions, even those not yet discovered (e.g., genetic engineering, nanotechnology, etc.).
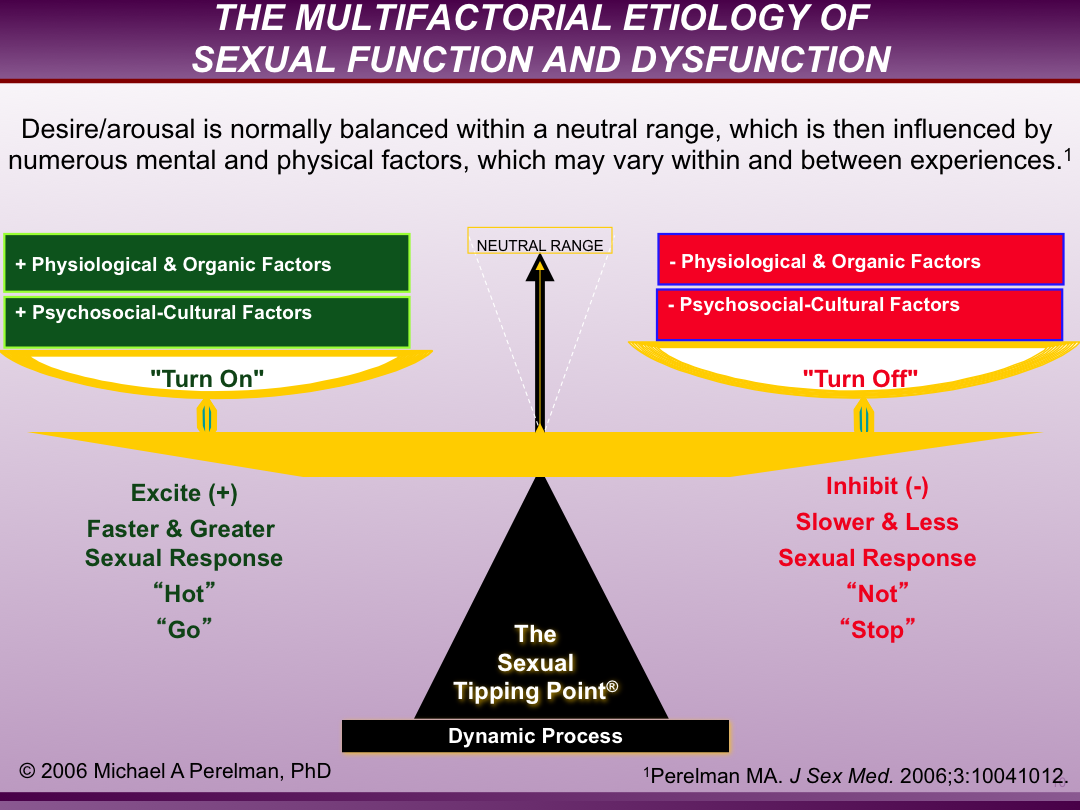
At the time the STP was first trademarked, it only partially resembled its current design as can be seen in these illustrations below from 2006.
Following more than a decade of presentations and publications on the STP model, in 2012, I presented the history of the various STP illustrations over the years in an invited address to The 15th World Meeting Of The International Society For Sexual Medicine (ISSM). A poster illuminating these different cartoons of the concept can be found on the mapedfund.org website under “History of STP Model.”
In 2012 I assigned the trademark registration to the not-for-profit MAP Education & Research Fund, Inc. That Foundation [a 501(3)(c) public charity] was founded] in 2011 with the mission of educating healthcare providers that sexual health is more than just biology. As a clinician, I felt it was critical to advance a model that would help students, professionals and the public alike understand that sex is always both mental and physical. Despite inadequate and/or nonexistent sex education in medical school, patients (who also often lack such education) are repeatedly told by media advertisements to “speak to your doctor about your sexual concerns." Most physicians however are poorly equipped to understand and treat sexual problems, beyond prescribing the most current medications. Additionally, most healthcare professionals are not comfortable discussing sexual matters with their patients, nor are they typically inclined to treat what are often misconstrued as “mere lifestyle problems." Instead, our media presents a sexually oversaturated society, which promotes unrealistic expectations, and misinformation resulting in more unnecessary suffering. Mapedfund.org launched as 2015 drew to a close. Copies of a Sexual Tipping Point® video animation, and related publications and presentations are available free from that website.
REFERENCES
Althof, S. E., Rubio-Aurioles, E., Perelman, M. A., & Rosen, RC (2012). Standard Operating Procedures for Taking a Sexual History. The Journal of Sexual Medicine, 10(1), 26–35
Althof, S. E. (2003). Therapeutic weaving: the integration of treatment techniques. In S. B. Levine (Ed.), Handbook of Clinical Sexuality for Mental Health Professionals (pp. 359–376). New York: Brunner-Routledge.
Althof, S. E., & Needle, R. (2008). The biopsychosocial evaluation of erectile dysfunction. In C. Carson, R. Kirby, & M. Wylie (Eds.), Textbook of Erectile Dysfunction (2nd ed.). New York: Informa.
Althof, S. E. (2006). Sexual therapy in the age of pharmacotherapy. Annual Review of Sex Research, 17, 116–131.
Bancroft, J., Graham, C. A., Janssen, E., & Sanders, S. A. (2009). The Dual Control Model: Current Status and Future Directions. The Journal of Sex Research, 42(2), 121–142.
Bancroft, J., Herbenick, D., Barnes, T., Hallam-Jones, R., Wylie, K. R., & Janssen, E. (2005). The relevance of the dual control model to male sexual dysfunction: the Kinsey Institute/BASRT collaborative project. Sexual & Relationship Therapy, 20(1), 13–30.
Bancroft, J. (1999). Central inhibition of sexual response in the male: a theoretical perspective. Neurosci Biobehav Rev, 23(6), 763–784.
Kaplan, H. S. (1974). The New Sex Therapy. New York: Brunner/Mazel.
Kaplan, HS & Perelman, M. A. (1979). The Physician and the Treatment of Sexual Dysfunctions. In G. Usdin & J. M. Lewis (Eds.), Psychiatry in General Medical Practice (pp. 1–27). McGraw-Hill Book Company.
Kaplan, H. S. (1995). The Sexual Desire Disorders: Dysfunctional Regulation of Sexual Motivation. New York: Brunner/ Mazel, Inc.
Kupferman, I. (1991). Hypothalamus and limbic system motivation. In E. R. Kandel, J. H. Schwartz, & T. M. Jessell (Eds.), Principle of Neural Science (3rd ed.). New York: Elsevier.
SR Leiblum & RC Rosen [Eds:] Principles and Practice of Sex Therapy. (2000). Principles and Practice of Sex Therapy (3rd ed.). New York: Guilford Press.
Leiblum, SR [Ed] Principles and Practice of Sex Therapy. (2007). Principles and Practice of Sex Therapy (4th ed.). Eds: SR & RC Rosen New York: Guilford Press.
Masters, W., & Johnson, V. (1970). Human sexual inadequacy. Boston, MA: Little,
Brown.
Masters, W., Johnson, A., & Kolodny, L. (1979). Textbook of sexual medicine. Boston, MA: Little, Brown.
McCarthy, B. W. (2001). Relapse prevention strategies and techniques with erectile dysfunction. J Sex Marital Ther, 27(1), 1–8.
McCarthy, B. W., & Fucito, L. M. (2005). Integrating medication, realistic expectations, and therapeutic interventions in the treatment of male sexual dysfunction. Journal of Sex and Marital Therapy.
McCarthy, M., & McDonald, D. (2009). Psychobiosocial versus biomedical models of treatment: Semantics or substance. Sex Relat Ther, 24(30), 30–37.
Perelman, M. (1984). Rehabilitative sex therapy for organic impotence. In T. Segraves & E. Haeberle (Eds.), Emerging dimensions of sexology (pp. 181–188). New York, NY: Praeger.
Perelman, M. A. (2003). Sex coaching for physicians: combination treatment for patient and partner. International Journal of Impotence Research, 15 Suppl 5, S67–74.
Perelman, M. A. (2005) Combination therapy for sexual dysfunction: integrating sex therapy and pharmacotherapy. In R. Balon & R. T. Segraves (Eds.), Handbook of Sexual Dysfunction (pp. 13–41). Boca Raton: Taylor & Francis.
Perelman, M. A. (2005) Psychosocial evaluation and combination treatment of men with erectile dysfunction [Review]. Urologic Clinics of North America, 32, 431–445.
Perelman, M. A. (2005). Idiosyncratic Masturbation Patterns: A Key Unexplored Variable in the Treatment of Retarded Ejaculation by the Practicing Urologist. Journal of Urology, 173(4), 340.
Perelman, M. A. (2006). The Sexual Tipping Point: A model to conceptualize etiology, diagnosis & combination treatment of female & male sexual dysfunction. Journal of Sexual Medicine, 3(Suppl. 1), 52.
Perelman, M. A. (2006). A new combination treatment for premature ejaculation: a sex therapist's perspective. Journal of Sexual Medicine, 3(6), 1004–1012.
Perelman, M. A. (2008). Integrated sex therapy: A psychosocial-cultural perspective integrating behavioral, cognitive, and medical approaches. In C. C. Carson, R. S. Kirby, I. Goldstein, & M. G. Wyllie(Eds.), Textbook of erectile dysfunction (2nd ed., pp. 298–305). London, England: Informa Healthcare.
Perelman, M. A. (2009). The sexual tipping point: a mind/body model for sexual medicine. Journal of Sexual Medicine, 6(3), 227–632.
Perelman, M. A., (2012). Sexual Balance: The Universal Versatility of the Sexual Tipping Point Model (JSM, Vol. 9, p. 266). Presented at the World Meeting On Sexual Medicine: The 18th Scientific Meeting Of The Sexual Medicine Society Of North America (SMSNA) And The 15th World Meeting Of The International Society For Sexual Medicine (ISSM).
Perelman, M. A. (2012). Helen Singer Kaplan's Legacy- Future of Sexual Medicine. Presented at the World Meeting On Sexual Medicine: The 18th Scientific Meeting Of The Sexual Medicine Society Of North America (SMSNA) And The 15th World Meeting Of The International Society For Sexual Medicine (ISSM).
Perelman, M. A. (2014). The history of sexual medicine. In APA Handbook of Sexuality and Psychology, Vol. 2: Contextual Approaches (pp. 137–179). Washington: American Psychological Association.
Perelman, M. A. (2015). Advocating For a Transdisciplinary Perspective in Sexual Medicine. Current Sexual Health Reports, 7(1), 1–2.
Pfaus J. Pathways of sexual desire. Journal of Sexual Medicine. 2009; 6(6):1506-1533.
Rosen, R. C., & Leiblum, S. R. (Eds.). (1989). Principles and practice of sex therapy. New York, NY: Guilford Press.
Rosen, R. (2000). Medical and psychological interventions for erectile dysfunction: Toward a combined treatment approach. In S. Leiblum & R. Rosen (Eds.), Principles and practice of sex therapy (3rd ed., pp. 276–304). New York, NY: Guilford Press.
Rosen RC, Miner, MM, Wincze JP. Erectile dysfunction: integration of medical and psychological approaches. In: Binik YM & Hall KSK, editors. Principles and practice of sex therapy, 5th edition. New York. Guilford Press. 2014.